
As an essential part of our lives, food is significant in building health for both people and the planet. Food not only provides nourishment, comfort, healing and a link to cultural identity for patients, it also provides opportunities to create sustainable and resilient communities.
Food is therefore an essential tool in addressing individual health, societal issues and environmental concerns. Unfortunately our current food paradigm is a central driver of our interlinked health, climate, and ecological crises.
The typical Western diet with its heavy reliance on animal and processed foods, and insufficient whole plant foods, is driving our epidemic of non-communicable diseases globally. The current level of chronic disease and its management are simply not sustainable, as evidenced by our burgeoning healthcare costs individually and as a society. According to the Global Burden of Disease Study, suboptimal diet is responsible for more deaths globally than any other risks, including tobacco, with most of these deaths due to cardiovascular disease, followed by cancer and type 2 diabetes (1). Improvement of diet could potentially prevent 1 in 5 deaths. Top dietary risks identified were high intake of sodium (reflecting our reliance on processed food), and low intake of whole grains, fruits, nuts and seeds, and vegetables. Clinical and country specific guidelines are now catching up to the medical literature and are incorporating plant-based diets into clinical practice guidelines for the prevention and management of chronic disease. The 2019 Canada Food Guide is an excellent example of this, with its food plate being at least 87.5% plant-based. Greater adherence to the Canada Food guide has been shown to significantly reduce the risk of cardiovascular disease (2).
The position statement on vegetarian diets by the Academy of Nutrition and Dietetics states that appropriately planned vegetarian, including vegan, diets are healthful, nutritionally adequate, and may provide health benefits for the prevention and treatment of certain diseases (3). These diets are appropriate for all stages of the life cycle, including pregnancy, lactation, infancy, childhood, adolescence, older adulthood, and for athletes. They note that vegetarians and vegans are at reduced risk of certain health conditions, including ischemic heart disease, type 2 diabetes, hypertension, certain types of cancer, and obesity.
Promoting plant-based nutrition at all stages of life can help prevent, manage and in some cases reverse non communicable diseases and support a more equitable and sustainable health system.
Animal agriculture is the leading cause of antibiotic resistance, which has been declared one of the top ten public health threats facing humanity by WHO. It is a leading cause of death, associated with close to 5 million annual deaths globally.
In 2018, an estimated 14,000 Canadian deaths were associated with antimicrobial resistant bacteria and cost our healthcare system $1.4 billion (4). Most antibiotics in Canada are used at farms not hospitals. In 2020, 82% of antimicrobials were sold for use in production animals, 17% for people, < 1% for cats and dogs and < 1% for plants/crops. Medically important antimicrobials sold for use in production animals in Canada is 3 times the quantity reported by European countries. (Canadian Antimicrobial Resistance Surveillance System (CARSS) Report 2022). Pandemic risk is another alarming bi-product of our industrialized food system, with ongoing global outbreaks of swine and bird flus, requiring culling of millions of animals in attempts to limit spread of the infectious diseases (5).
Global food production is responsible for 35% of all greenhouse gas emissions (GHGE), with the use of animals as a source for food, as well as feed for farmed animals, responsible for almost 60% of all food production emissions. Seminal research by Poore and Nemecek (2018) which compiled data from life cycle assessments in 570 published papers covering 38,700 commercial farms across 119 countries, representing 90% of all food products, showed that beef and dairy had the greatest GHGE and land use impact (6).
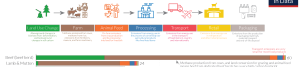
A global shift to a plant-based diet would reduce GHGE from food by about 50%. Eliminating beef alone would reduce GHGE by 33%. Even the lowest-impact animal products have a much higher impact than plant sources of protein. Of note, about 85% of GHGE is at the production phase, so while buying local is important, which food we choose to eat is far more impactful in reducing our climate footprint.

To have any hope of meeting the central goal of the Paris Agreement, which is to limit global warming to 2°C or less, our carbon emissions must be reduced considerably, including those coming from agriculture. Clark et al. show that even if fossil fuel emissions were eliminated immediately, emissions from the global food system alone would make it impossible to limit warming to 1.5°C and difficult even to realize the 2°C target (7). Thus, major changes in how food is produced are needed if we want to meet the goals of the Paris Agreement.
Although we often focus on GHGE, the global food system, particularly animal agriculture, has a broader impact on planetary health (8). Animal agriculture is the biggest driver of wildlife and biodiversity loss, species extinction, freshwater use, water pollution and ocean destruction (9).
Half of all habitable land is used for agriculture, 80% of which is used for animal agriculture which only supplies 18% of global calories. Land use change, mainly land conversion for crop production, raising farmed animals and plantations is the strongest driver of our destruction of nature. Transitioning to a plant-based food system will free up to 75% of land that can be used for rewilding (10).

In 2019 the Eat Lancet commission produced their landmark work with the global planetary health diet, a reference diet that will keep the food system within planetary boundaries whilst improving human health and preventing an estimated 11 million deaths globally per year. It is a predominantly plant-based diet with animal foods considered to be optional and if consumed, contributing about 13% of energy intake (11).
The single biggest lever we can use as individuals and institutions, for individual health and to mitigate planetary destruction, is to promote plant-based nutrition at all levels including for our in-patient hospital food, in our canteens and food services, at our conferences, rounds, and healthcare events (12,13,14,15,16). The latest IPCC report states ‘reduction of excess meat consumption is amongst the most effective measures to mitigate GHG emissions with a high potential for environmental health, food security, biodiversity and animal welfare co-benefits’. Healthcare professionals and systems have a powerful opportunity to be leaders in nourishing the health of their people and the planet on which we depend (17, 18, 19).
Learn with us!
The way our food is produced, processed, consumed and wasted has profound impacts on environmental, public and human health. Approximately 71% of the global health care footprint stems from the production, transport and disposal of goods and services – including food (1). As anchor institutions, health care organizations have the power to assert procurement standards that support local and sustainable food systems resulting in social, economic and environmental benefits for communities. By sourcing locally, institutions not only reduce emissions and the environmental impact of food procurement, they also support the local economy (2).
Coalition Resources
- Local Food for Ontario Hospitals
- Report on Food Provision in Ontario Hospitals and Long-TermCare Facilities: The challenges and opportunities of incorporting local foods
- Local Food Provision in Ontario’s Hospitals and Long-term Care Facilities: Recommendations for stakeholders
- Healthy Sustainable Food Procurement: Making the case for health care engagement
- Assessing opportunities for Local food in Health Care
- Healthy Food in Health Care: A pledge for fresh, local sustainable food
- Local Food Background Guide
External resources
Sustainable menus feature low emission foods and plant-rich diet options that optimize nutrition. These menus encourage climate smart eating, which involves producing and consuming foods that minimize its impact on the environment.
Plant-rich diets not only hold potential for climate change mitigations and reduced environmental impacts, they also tend to be healthier and have shown to result in significant cost savings.
External resources
Approximately one-third of the world’s food is never eaten, accounting for almost 8% of global greenhouse gas emissions (1). In a hospital setting an average 10-15% of waste generated is food (2).
Not only is this a loss of economic resources for health care organisations but it is also a waste of wider environmental resources . By reducing food waste we can reduce the need for resources used to produce food and thus reduce the emissions released in the process (3).
One way to reduce food waste in health care is through the offering of menus and room service. The transition to this system of food management has also been shown to result in cost savings and increased patient satisfaction (4).
To help reduce the environmental impact of wasted food, we can look at different forms of food waste management. Organic waste in landfills generate potent greenhouse gasses, when alternative methods of disposal are utilized, such as composting, the resulting emissions are significantly reduced (5). There are a variety of potential landfill alternatives, including: on-site composting, off-site composting, and food scrap donation. What works best for a facility will vary according to size and volume of food waste generated.
Coalition Resources
External Resources
Our Projects

This Business Case and Implementation Guide outline why health care facilities need to prioritize the transformation of their food services and how they can implement a sustainable food service model through embracing food as medicine, reducing food waste, implementing plant-forward menus and shifting to values-based procurement for food.
These actions present a clear path toward both improved patient care and environmental sustainability.
Read it HERE.
Purpose and Scope
The Sustainable Food Services Committee is a working group that provides implementation advice, strategies, and research to support hospitals and other health care institutions in implementing sustainable menu choices including: plant forward menus, values-based procurement practices, viewing food as medicine, and food waste reduction.
The committee primarily focused on Ontario health care, with some work on a national scale.
Meetings happen once every two months.
If you are interested in joining, please contact us at parascf@mcmaster.ca.
Project SOIL (Shared Opportunities on Institutional Lands), funded by the New Directions Research Program, Ontario Ministry of Agriculture, Food and Rural Affairs, was feasibility study that explored the potential of on-site food production for public institutions through arrangements with local producers, particularly where access to farmland is limited and expensive.
This project involved results of visioning sessions undertaken in 2016 with five institutions, to further gauge the potential of on-site food growing projects and gain insights to expand this approach. Each case summary includes details on initial interest, identification of possible barriers and responses, development of information on models, building connections with local producers, and sharing resources. Co-benefits identified include community engagement on local food production, health and wellbeing, job creation and training opportunities, patient rehabilitation programs and generation of funds needed to foster these types of programs.
Results: SOIL Final Report
From October to March 2011, Ross Memorial Hospital (RMH) and project partners with funding from the Broader Public Investment Sector Fund, worked with food distributors to improve the availability of local food options. This was of benefit to RMH, and the entire Region of the City of Kawartha Lakes. The goal of the project was to promote local food by developing new and local menu items at RMH and evaluate the impact that serving local food has on patient satisfaction and food waste.
Results: Local Food Case Study #3: Ross Memorial Hospital decreases ecological footprint with wholesome, nutritious local food
Partners:
- Health Care: Ross Memorial Hospital, Lindsay, ON
- Business: Sysco Central Ontario
- Academic: Dr. Mustafa Koc, Ryerson University – Project Advisor, Dr. Paulette Padanyi, University of Guelph – Project Advisor
- Non-Profit and Community: City of Kawartha Lakes, Canadian Coalition for Green Health Care, My Sustainable Canada
According to a Canadian Coalition of Green Health Care survey conducted jointly with My Sustainable Canada and funded by the Ontario Trillium Foundation, several Ontario health care facilities were purchasing local food, but none had undertaken extensive food service audits. These audits could provide baseline information on the quantity of Ontario food served in the health care sector. Food origin audits could also enhance the capacity for Ontario food to enter the health care supply chain by identifying all foods that are sourced from outside Ontario, but are available locally. Furthermore, there were no known systems in place to monitor local food purchasing among health care facilities and group purchasing organizations in Ontario.
From February – December 2011, with funding from the Broader Public Investment Sector Fund, YMCA Youth Eco Internship Program, the Coalition and partners conducted food origin audits at one health care facility and its Group Purchasing Organization (GPO) by: documenting the origin of foods purchased by this facility; identifying opportunities for it to purchase Ontario food; and, outline which food products have a reasonable ready supply for this organization to start/increase its purchase of Ontario foods.
The goal of this project was to create a set of best practices for conducting food origin audits that identify the origin and measure current food purchases among the health care food services sector; establish a process for increased collaboration and partnerships between the agri-food sector and the health care value chain; increase the quantity and percentage of Ontario food products purchased by members of the health care value chain; and share results with members of the health care food services sector, including the broader public sector value chain.
Results:
- Conducting Food Origin Audits: a step-by-step guide. Do you know where your food comes from?
Download English PDF >> or French PDF >> - Local Food Case Study #1 – St. Joseph’s Health Centre Guelph
Download English PDF >> or French PDF >> - Local Food Case Study #2 – St. Joseph’s Group Purchasing Organisation
Download English PDF >> or French PDF >> - April 20, 2011 Workshop – Local Food in the Public Sector: A Perspective for Health Care
- Agenda (pdf), Backgrounder (pdf), PowerPoint Presentations: Presentation 1 (pptx), Presentation 2 (pptx), Presentation 3 (ppt), Pictures
This project was developed From July 2009 – August 2010, the Coalition was funded by the Ontario Trillium Foundation, YMCA Youth Eco Internship Program, to study the practicality, cost benefit, health and environmental benefits of incorporating local food into patient meals and cafeterias. During the course of the project 50 hospitals and long term care facilities were administered a survey, with 33/50 responding; a webinar was presented on the results of the survey; an information session was presented on the opportunities to introduce local food into health care; established increased collaboration with local food professionals, vendors, and supply chains Identified; the Coalition also identified 1-2 hospitals interested in local food pilot project.
Results:
Resources
- UHN Food Ecosystem
- Healthy People, Healthy Planet
- CASCADES – Sustainable Foods Infographic
- EcoFood Guide
- Future 50 Foods
- EAT-Lancet Commission Brief for Healthcare Professionals
- The Role of Dietitians in Sustainable Food Systems and Sustainable Diets from the Dietitians of Canada
- Eating patterns for health and environmental sustainability : a reference guide for dieticians from the British Dietetic Association (BDA)
- Cascades Food Infrastructures for Planetary Health Playbook



